Eye Tumor
Topics:
• Choroidal Hemangioma• Choroidal Melanoma
• Choroidal Metastasis
• Choroidal Nevus
• Conjuctival Tumors
• Eyelid Tumors
• Iris Tumors
• Lymphoma/Leukemia
• Melanocytoma
• Orbital Tumors
• Retinoblastoma
Choroidal Hemangioma
Many choroidal hemangiomas can be safely monitored by your eye doctor without the need of further treatment. Photographs can be used to document evidence of growth or leakage and the need for treatment. Treatment options may include photodynamic therapy, laser photocoagulation to decrease the amount of fluid leakage, or low doses of external beam radiation therapy.
Choroidal Melanoma
A choroidal melanoma is malignant, meaning that the cancer may metastasize and eventually spread to other parts of the body. Because choroidal melanoma is intraocular and not usually visible, patients with this disease often do not recognize its presence until the tumor grows to a size that impairs vision by obstruction, retinal detachment, hemorrhage, or other complication. Pain is unusual, except with large tumors. Periodic retinal examination through a dilated pupil is the best means of early detection.
Cutting out the tumor and leaving the rest of the eye is not routinely advised for this type of cancer. Opening the eye during surgery would allow the tumor cells to float around into the spaces around the eye, which could spread cancer cells to other parts of the eye. In addition, some studies have shown that up to 50% of choroidal melanomas invade the sclera. Therefore if the tumor is removed from the eye there is a high possibility that cancer cells will remain within the sclera. Lastly, many eyes do not tolerate this procedure and severe complications may occur such as detachments of the retina, hemorrhages, and recurrence of the tumor which may result in having to remove the eye anyway.
Treatment recommendations for choroidal melanoma usually are based on the size of the tumor. Small suspicious melanomas usually are closely watched for evidence of growth before treatment is recommended. Medium-size tumors may be treated with either radioactive plaque therapy or enucleation (removal) of the eye. The Collaborative Ocular Melanoma Study (COMS), supported by the National Eye Institute of the National Institutes of Health, has documented equal success rates for plaque radiation therapy or enucleation for preventing the spread of cancer. Large-size tumors usually are best treated by enucleation. This is because the amount of radiation required to treat the tumor is too much for the eye to tolerate. The COMS study found no benefit to large-size tumor patients having radiation therapy prior to enucleation.
Choroidal Metastasis
Malignant tumors from other parts of the body can spread in and around the eye. Metastatic cancers that appear in the eye usually come from a primary cancer of the breast in women and the lungs in men. Other, less common, sites of origin include the prostate, kidneys, thyroid, and the gastrointestinal tract. Blood cell tumors (lymphomas and leukemia) also can spread to the eye. The care of patients with metastasis to the eye should be coordinated between the eye cancer specialist, medical oncologist, and radiation oncologist. Treatment options may include chemotherapy, external beam radiation therapy, or, more rarely, enucleation.
Choroidal Nevus
Like a raised freckle on the skin, a nevus can occur inside the eye. And, like a skin nevus, a choroidal freckle can become malignant, so should be closely monitored. A choroidal nevus should be examined by an ophthalmologist every four to six months to check if the pigmentation or size of the nevus has changed. In most cases, the only treatment recommended is close observation and monitoring by an ocular oncologist.
Conjunctival Tumors
Conjunctival tumors are malignant cancers that grow on the outer surface of the eye. The most common types of conjunctival tumors are squamous cell carcinoma, malignant melanoma, and lymphoma. Squamous cell carcinomas rarely metastasize, but can invade the area around the eye into the orbit and sinuses. Malignant melanomas can start as a nevus (freckle) or can arise as newly formed pigmentation. Lymphoma of the eye can be a sign of systemic lymphoma or be confined to the conjunctiva.
Both squamous cell carcinomas and malignant conjunctival melanomas should be removed. Most small conjunctival tumors can be photographed and followed for evidence of growth prior to treatment. Small tumors can be completely removed surgically. In other instances cryotherapy (freezing therapy) may be necessaryor chemotherapy eye drops may be used to treat the entire surface of the eye.
Eyelid Tumors
Tumors of the eyelid may be benign cysts, inflammation, or malignant skin cancers. The most common type of eyelid cancer is basal cell carcinoma. Most basal cell carcinomas can be removed with surgery. If left untreated, these tumors can grow around the eye and into the orbit, sinuses and brain. A simple biopsy can determine if an eyelid tumor is malignant. Malignant tumors are completely removed and the eyelid is repaired using plastic surgery techniques. Additional cryotherapy (freezing-therapy) and radiation therapy sometimes are required after surgery.
Iris Tumors
Tumors can grow within and behind the iris. Though many iris tumors are cysts or a nevus, malignant melanomas can occur in this area. Most pigmented iris tumors do not grow. They are photographed and monitored with a special slit lamp and high frequency ultrasound to establish a baseline for future comparisons. When an iris tumor is documented to grow, treatment is recommended. Most small iris melanomas can be surgically removed. Radiation plaque therapy or enucleation may be considered for larger iris tumors.
Lymphoma/Leukemia
Lymphoma tumors can appear in the eyelid tissue, tear ducts and the eye itself. In most patients with large cell non-Hodgkin's lymphoma, the disease is confined to the eye and central nervous system. In these patients, symptoms appear in the eye an average of two years before they are seen elsewhere. The disease itself as well as treatment, which may include external beam radiation, chemotherapy, or both (chemoradiation) to the central nervous system, can affect visual functioning.
Melanocytoma
This extremely slow-growing tumor usually is found on the surface of the optic disc. Almost all cases of melanocytoma are benign and malignant transformation is rare. It is probably present at birth and typically, there are no symptoms. Under clinical examination and fluorescein angiographic studies, melanocytoma appears as a deeply pigmented area located over the optic disc. In the majority of cases, close observation is recommended and no treatment is required. If malignant transformation does occur, enucleation, may be considered.
Orbital Tumors
Tumors and inflammations can occur behind the eye. These tumors often push the eye forward causing a bulging of the eye called proptosis. The most common causes of proptosis are thyroid eye disease and lymphoid tumors. Other tumors include hemangiomas (blood vessel tumors), lachrymal (tear) gland tumors, and growths that extend from the sinuses into the orbit. Though CT scans, MRI's and ultrasounds help in determining the probable diagnosis, most orbital tumors are diagnosed by a biopsy.
When possible, orbital tumors are totally removed. If they cannot be removed or if removal will cause too much damage to other important structures around the eye, a piece of tumor may be removed and sent for evaluation. If a tumor cannot be removed during surgery, most orbital tumors can be treated with external beam radiation therapy. Certain rare orbital tumors may require removal of the eye and orbital contents. In certain cases, orbital radiotherapy may be used to treat any residual tumor.
Retinoblastoma
We all know that life is always not fair and that there are no guarantees. This becomes painfully evident when a child is diagnosed with cancer.
There are two types of retinoblastoma. Familial retinoblastoma is hereditary, is passed from parent to child, and is bilateral (affects both eyes). Familial retinoblastoma represents 10% of cases. It is associated with a long-term predisposition to other types of cancer. The second type of retinoblastoma, responsible for 70% of all new cases, is unilateral (only one eye is affected). It represents the non-heritable form of the disease, and carries no increased risk of a second tumor.
Ninety percent of all retinoblastoma cases are diagnosed within the first three years of the child's life. On average, children with familial retinoblastoma typically are diagnosed at four months of age. When there is no family connection, the cancer is usually diagnosed when the child is approximately one to two years of age.
Well Baby Screening
- The Red Reflex: checks for a normal red reflection in the eye that occurs when light travels inside the eye, hits the retina and the blood tissue, and is reflected back.
- The Corneal Light Reflex: when a light is shined into each cornea a symmetrical beam of light is reflected back in the same spot on each eye. This helps to determine whether the eyes are crossed.
- An Eye Examination: to check for any structural abnormalities. From six to twelve months of age, the eyes' ability to fix and follow objects both individually and together is evaluated. Between the ages of three and five, the examination of the eyes is coupled with testing for visual acuity, color vision and depth perception.
Parents also may want to look for eye abnormalities by directly examining each of the child's eyes under good lighting conditions. Both eyes should appear equal in size, be aligned, and should be able to move together and focus forward. Parents can observe the red reflex can be seen by dimming the room lights and using a flashlight to shine light directly into the child's eyes.
Unfortunately, because retinoblastoma is a rare cancer, some pediatricians may fail to detect it early enough or sometimes mistakenly diagnose it as:
- Persistent hyperplastic primary vitreous (PHPV): an unusual congenital anomaly whereby the eye is shorter than normal, develops a cataract, and may present with whitening of the pupil.
- Coat's disease: a typically unilateral disease, affecting young boys, leading to blood vessel abnormalities in the retina and retinal detachment.
- Toxocara canis: an infectious disease of the eye associated with exposure to infected puppies. This infection causes a retinal lesion leading to retinal detachment, which can mimic retinoblastoma.
- Retinopathy of prematurity (ROP): involves damage to the retinal tissue. It is associated with low birth weight infants who receive supplemental oxygen in the period immediately after birth.
Signs and Symptoms

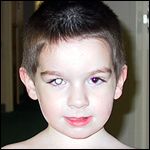
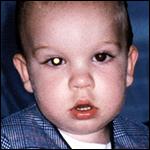
Leukocoria is the most common sign of retinoblastoma and can be seen in 60% of patients. Other signs may include strabismus or crossing of the eyes, which is noticed in 20% of children. Furthermore, in approximately 10% of children, eye swelling with pain and redness occurs. (Photo of leukocoria)
It is extremely important that a child suspected of having retinoblastoma be evaluated by a team of specialists, including an ocular oncologist, a pediatric ophthalmologist, a radiation oncologist, and a pediatric oncologist within an ocular oncology center. Children with this rare cancer require the most advanced testing and management to ensure the cure of the cancer with preservation of the greatest amount of vision. Specialized testing is very important to confirm diagnosis, as there are no blood tests available to confirm a diagnosis of retinoblastoma. Unlike tumors in other parts of the body, a biopsy cannot be performed due to the risk of spreading cancer cells outside the eye.
The Initial Eye Exam
Before the ophthalmologist examines your child, an optometrist or ophthalmic technician may take a medical and family history. Your child will receive eye drops that will dilate the pupils of the eye, which allows the ophthalmologist to examine the interior of the eye. The ophthalmologist will discuss his initial findings and possible treatment options.
The doctor may recommend an Examination Under Anesthesia (EUA) and any possible procedures that may be necessary during the EUA. Before the EUA a routine blood sample will be obtained to evaluate the components of the blood. Blood is obtained by a small prick made in a fingertip and a few drops are drawn off. If any of the tests are abnormal, more tests may be necessary to find out the reason. Tests may be performed to measure:
- Hemoglobin: the substance in the red blood cells that carries oxygen and is responsible for the blood's red color. Lower hemoglobin amounts than indicate anemia.
- Hematocrit: a measure of the amount of red blood cells, expressed as a percentage of the whole blood that is made up of red cells. A low count may indicate anemia.
- Platelets: the component of the blood that helps stop bleeding in case of injury.
- White Blood Cell Count (WBC): the components of blood that fight infection. Children receiving chemotherapy generally have a lower white cell count than normal.
Specialized Testing
Imaging Studies
- Computerized Tomography (CT): A CT scan of the head is a computerized X-ray that provides a very clear picture of the eyes, the surrounding tissue and the brain. During the scan, the child's head is placed on a special headrest to allow proper positioning and to minimize movement during the scanning procedure. Unlike an ordinary X-ray machine, which takes one picture at a time, the CT scanner takes a number of small pictures as it rotates around the patient. This procedure takes about one hour.
- Magnetic Resonance Imaging (MRI): Magnetic Resonance Imaging uses magnetic fields and radio waves linked to a computer to create pictures of areas inside the body. The child lies on a table that slides into a tunnel-shaped piece of equipment. Antennas within the MRI machine pick up the radio waves within and feed them into a computer that assembles a picture. Because MRI can "see" through bone, it can provide clearer pictures of tumor located near bone and in the orbit. This procedure also takes about one hour.
Ultrasound (Echography)
 During an ultrasound examination sound waves are directed towards the tumor by a small probe
placed on the eye. Because tumors generate different "echoes" than normal tissue, sound waves above the range of
human hearing can be bounced off tissue and then changed electronically into images. The pattern made by reflection
of the sound waves helps to confirm that tumors are present and assists the doctor in establishing what type of tumor
is present. Ultrasound also helps to determine the thickness or height of the tumor.
During an ultrasound examination sound waves are directed towards the tumor by a small probe
placed on the eye. Because tumors generate different "echoes" than normal tissue, sound waves above the range of
human hearing can be bounced off tissue and then changed electronically into images. The pattern made by reflection
of the sound waves helps to confirm that tumors are present and assists the doctor in establishing what type of tumor
is present. Ultrasound also helps to determine the thickness or height of the tumor.Bone Marrow and Lumbar Puncture
Bone marrow is the substance inside the larger bones of the body where healthy new blood cells are made. A small amount of the bone marrow is removed from the hip through a small needle and examined in the laboratory for cancerous cells. Since retinoblastoma can also spread into the brain, tumor cells may be floating in the cerebral spinal fluid (CSF) that bathes the brain and the spinal column (inside the backbone). To obtain the CSF, a small amount of fluid is drawn through a narrow needle at the base of the spine. The CSF is then tested for cancerous cells.